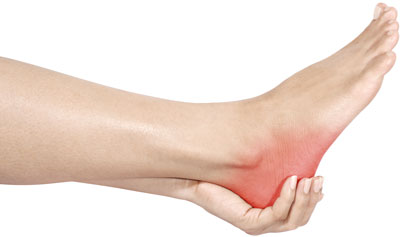
Plantar fasciitis is one of the most commonly treated types of foot pain in physical therapy. Overuse or repetitive stress to the bottom aspect of the foot is the most common cause. It typically affects younger females however males are also likely to have symptoms. Older individuals are at risk for developing plantar fasciitis as well as athletes. Individuals with an elevated body mass index are prone to heel pain and other foot conditions. Typically symptoms of plantar fasciitis will include pain on the bottom of the foot upon standing after prolonged inactivity or after an increase in activity. This is common when runners increase their distances. Symptoms may include chronic heel pain leading up to plantar fasciitis or chronic calf tightness.
What is Plantar Fasciitis?
The plantar fascia is a thick band of connective tissue that spans the bottom of the foot. It runs from the calcaneus (heel bone) down towards the toes. The plantar fascia assists in walking by providing stability to the ankle and foot. In cases of plantar fasciitis, the tissue is “overloaded”. This may cause pain that is most pronounced when standing for prolonged periods of time or upon standing after prolonged sitting. Chronic calf tightness or flat feet may be risk factors for developing plantar fasciitis. However, any activity that increases the force on this structure may cause symptoms.
What can a Physical Therapist do for you?
Techniques utilized by a physical therapist can significantly decrease plantar fasciitis related symptoms. Some of these techniques include manual therapy to increase the ankle range of motion. Improving ankle/foot range of motion through patient-specific exercise is also important. Your physical therapist may recommend exercises that reduce the load on the foot to start, including bike riding or swimming. Various athletic taping techniques have been proven to help reduce the load on the foot and allow the plantar fascia time to “rest”. These taping techniques have been shown to be an effective form of care in treating plantar fasciitis. Your physical therapist may also be able to assist you in an orthotic recommendation. Orthotics may be especially effective for individuals who respond well to taping techniques.
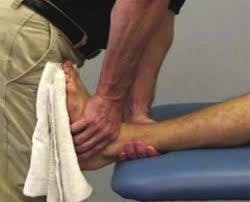
Balance exercises are incorporated as symptoms improve. Exercises to target hip and knee strength and range of motion impairments may also assist in improving symptoms. Calf and heel cord stretching is another effective method to reduce symptoms. These techniques will help progress a patient back to their sport or daily function without pain and allow for pain-free activity and improve your overall quality of life. Talk to your physical therapist to see if your plantar fasciitis symptoms can be alleviated by some of these treatment options.
Conclusion
Plantar fasciitis is a common form of foot pain that impacts many lives and limits function. Plantar fasciitis symptoms may resolve on its own over time, sometimes up to one year. However, treatment by a physical therapist may assist alleviating pain at a rapid pace. No one treatment works best for everyone. A physical therapist can assist you in determining the treatment plan that is going to be the most effective for you to reach your goals. There are many other forms of foot pain that may mimic plantar fasciitis. Your physical therapist can help in screening for these other types of injuries. Come to talk to your physical therapist today!
Written by Dr. Steve Ferro, PT, DPT, OCS
References
1.Martin R, Davenport T, Reishl, S, et al. Heel Pain–Plantar Fasciitis: Revision 2014. Journal of Orthopaedic & Sports Physical Therapy. 2014;44(11):A1-A33. DOI: 10.2519/jospt.2014.0303.
2.Cole C, Seto C, Gazewood J. Plantar fasciitis: evidence-based review of diagnosis and therapy. American Family Physician. 2005;72:2237–2242.
3.Pollack Y, Sashua K, Kalichman L. Manual therapy for plantar heel pain. The Foot. 2018;34:11-16. DOI: 10.1016/j.foot.2017.08.001.
4.Stecco C, Corradin N, Macchi V, et al. Plantar fascia anatomy and its relationship with Achilles tendon and paratenon. Journal of Anatomy. 2013;223(6):665-76. DOI: 10.1111/joa.12111.