As many as 9 in 10 competitive swimmers aged 13 to 25 years report shoulder pain. This is primarily due…

Your mother wasn’t joking when she told you to sit up straight! Recent research supports good posture and its effect…

Rounded shoulders are the norm in today’s society. We sit for long periods of the day, often staring at computer…

Chronic rotator cuff pain leads to the weakening of the 4 muscles and their tendons. The best exercises for rotator…
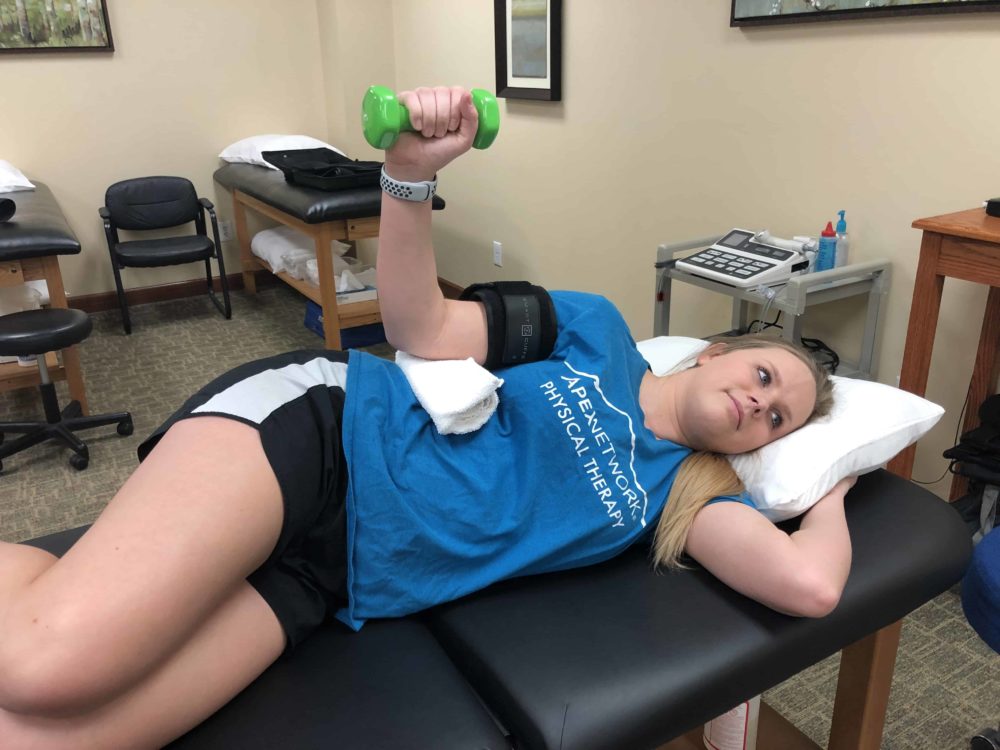
About 1 in 5 adults experience shoulder pain. Rotator cuff tendon pain is the most common type. If you are…

As many as 1 in 4 Americans experience shoulder pain. Pain ranges from a mild nuisance to severe disability. Shoulder…

Recovery from shoulder surgery is a long process. Soreness lasts anywhere from a few weeks to several months. During your…

Are you stretching your shoulders but not seeing any real improvement in your range of motion? Many people see little…

About half of people who suffer a shoulder dislocation will have a second dislocation within 2 years. Several types of…

Your shoulder is the most mobile joint in your body. However, it is also the most often dislocated joint. Shoulder…
