Do you suffer from pain on the outside of your knee? IT Band syndrome is one of the most common…
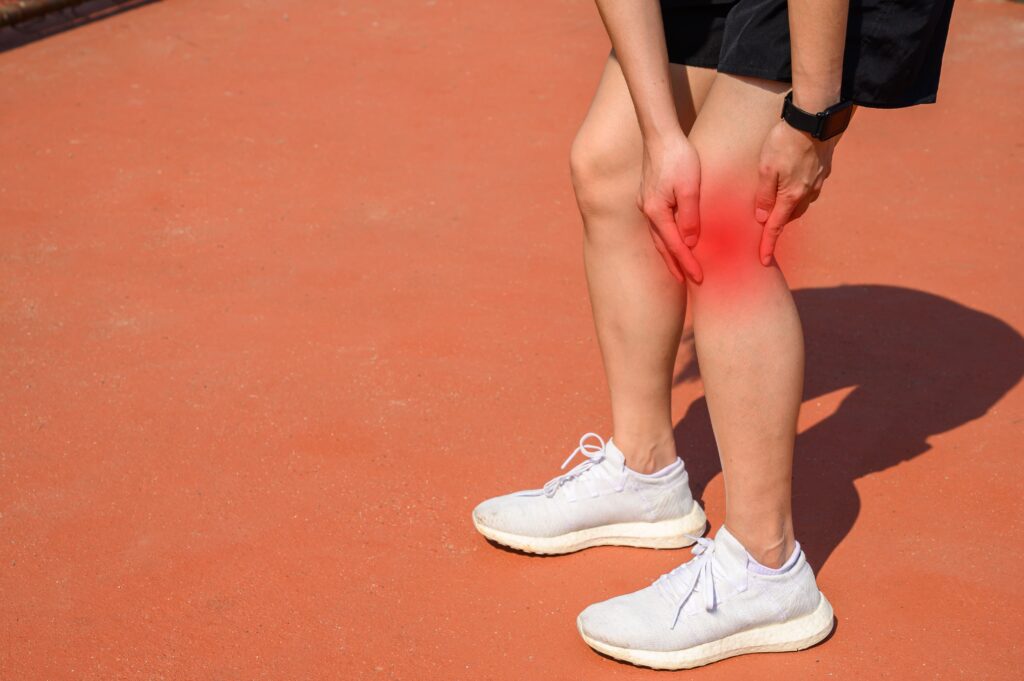
Knee pain from Osgood-Schlatter Disease affects 1 in 10 adolescent athletes. The hallmark sign is pain and swelling just below…

We know how frustrating pain from knee arthritis can be. Due to pain and lost mobility, each year hundreds of…

The primary focus of rehab programs for jumper’s knee is tendon loading exercises. These exercises require high muscle activation of…

Patellar tendinitis, also known as jumper’s knee, is a chronic problem for many athletes. Pain begins with a dull annoying…

Jumper’s knee, or patellar tendinitis, is common in basketball and volleyball players. Across all sports, up to 22% of elite…
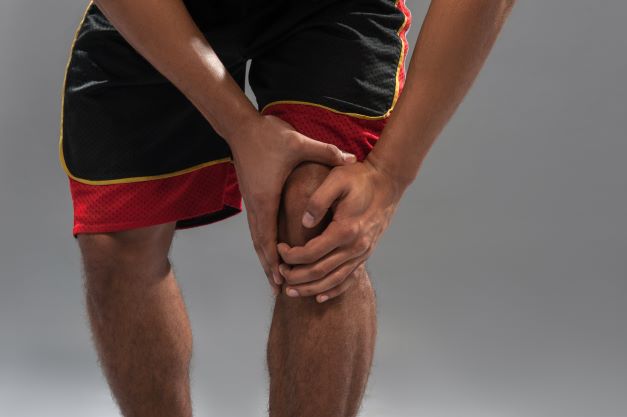
This year, 250,000 ACL injuries are estimated to occur in the U.S. Unfortunately, only 63% of athletes ever return to their sport after…

After ACL surgery, persistent quadriceps and hamstring weakness will delay your return to sport. Weakness of your injured leg will…
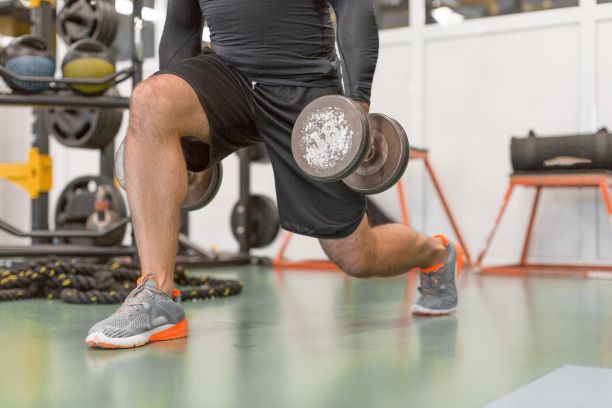
You are not guaranteed to return to your sport after your ACL reconstruction. 1/3 of athletes never return to their…

ACL rehab is a grind after surgery. Your recovery will be slow and full of ups and downs. Only 63%…
