Recent changes in health care have placed increased pressure on physical therapists to become more efficient and effective with their treatments. More so than ever, the diagnosis, treatment, and education of a patient must be done quickly and accurately in a limited number of treatment sessions. In order to practice in such an environment, physical therapists must possess adequate problem solving skills and be able to utilize knowledge within the decision making process. These attributes are believed to be present in expert health care professionals. However, expertise is a difficult term to define, let alone recognize in practice. In its most simplistic form, clinical expertise can be described as advanced skills and/or knowledge in a particular field. However, possessing these attributes alone do not guarantee expertise. Understanding how expert physical therapists practice has important implications for how patients interact and collaborate with their physical therapist.
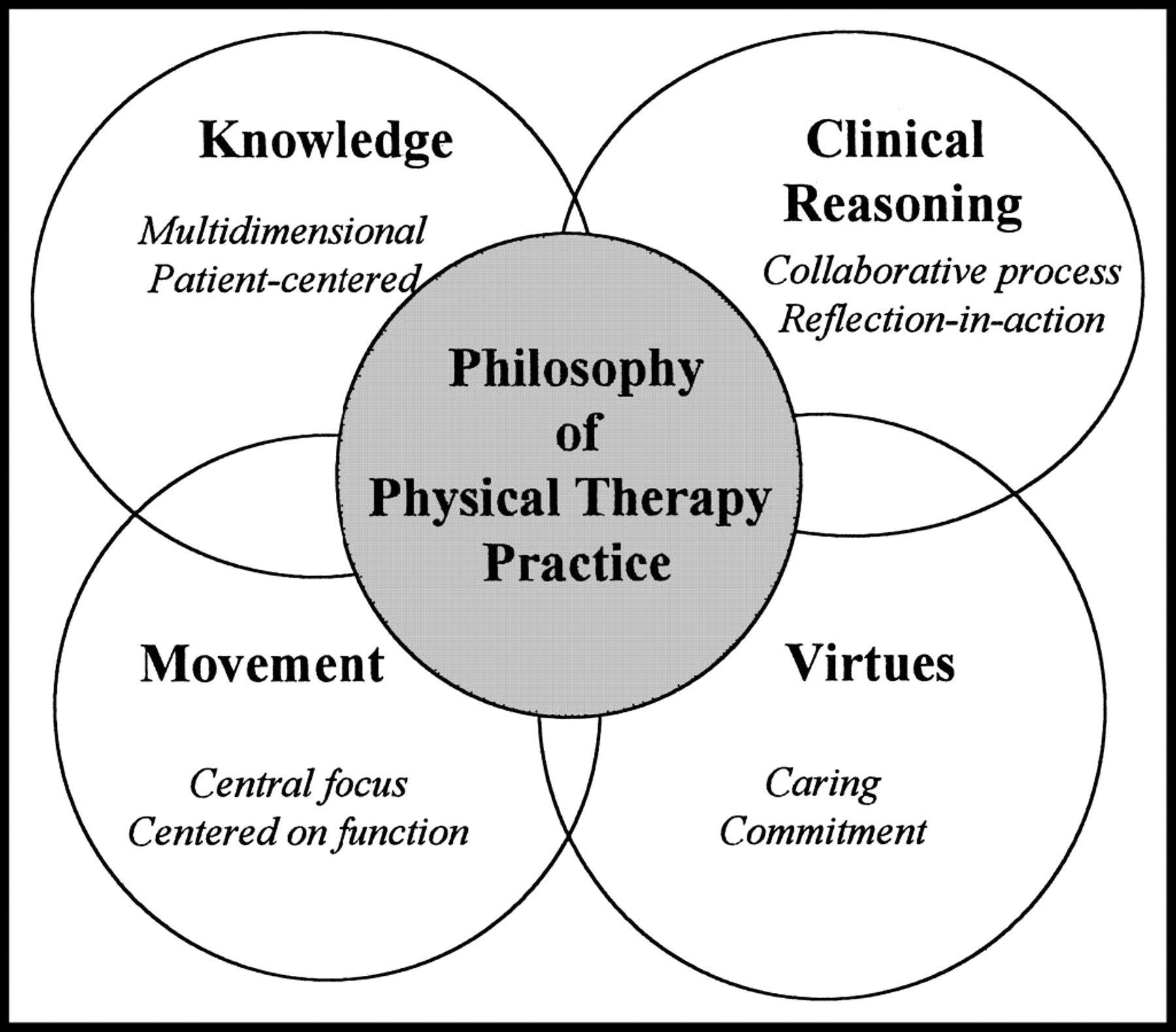
Jensen & Colleagues1 were the first to investigate the attributes of expert practice in physical therapy. The researchers identified four major dimensions of expert practice: knowledge, clinical reasoning, movement, and virtues. At the center of their proposed model is the idea that expert physical therapists viewed their practice as starting and ending with the patient (a patient-centered approach). Expert physical therapists make it a point to listen to, believe, and understand all their patient’s concerns and then collaborate with the patient to formulate a plan to regain function. Now, let’s further explore the four core dimensions of expert physical therapy practice.
Knowledge: Patient-Centered
Formal study such as academic degrees, advanced training, and other methods of self study are acknowledged as important components of lifelong learning in any field. However, expert physical therapists view their patients as the most important source of their knowledge. This is often exemplified through the essential practice of active listening. With active listening, the expert maintains eye contact, sits at the same level as the patient, and engages in focused interaction. Patients are allowed to tell their story instead of the physical therapist running down a list of questions that more closely resembles a prisoner interrogation instead of a true conversation. This allows the expert to not only understand the diagnosis but to also understand the patient as a person and how their problem is impacting their life. Experts also engage in a reflective process about their patients which further enhances learning and the storage of new clinical knowledge.
A Collaborative Process
Together with the patients, the expert physical therapist seeks to understand what the patient wants and expects from their therapist and how this fits into the context of their life. Once the patient and therapist have identified the problem(s), both must collaborate to problem solve. The therapist’s primary role is to educate the patient about movement and function. The treatment plan must make sense for the patient. The physical therapist should answer all questions until it does make sense. Effective treatment depends on the patient understanding their role and then following through. This enhances the likelihood that the patient will take control and be willing to modify behaviors and lifestyle factors necessary to regain function.
Movement as a Central Focus
Experts possess and utilize hands on skills when assessing patient’s functional movement and when engaged in treatment. They also assess movement through seeing with their eyes and feeling with their hands. Experts seem to unconsciously guide, facilitate, and reinforce a desired movement from their patients through touch and a therapeutic tone of voice. Experts rarely utilize equipment in the clinic or as part of a home program. Instead patients are instructed in exercises with guidance from the therapist’s hands while always relating the purpose back to the patient’s goals. Experts typically prescribe a few simple exercises specific to functional movements important to the patient.
Virtues: Caring & Commitment
Experts possess the personal attributes of caring and commitment. They are committed to doing what is best for the patient. Challenging patient cases or problems are exciting to these experts. Experts also communicate this sense of caring and commitment as evidenced by spending adequate time with the patient in the clinic and through other means of interactions (telephone, emails, etc).
Putting Expertise into Practice
The perceived greatest barrier to expert practice is time with the patient and the changing landscape of health care strengthens this threat. Physical therapists need time with their patients in the clinic and time to later reflect on their clinical practice. Under the right circumstances and in the right environment physical therapists and their patients can flourish. Important considerations to take advantage of the expertise of any physical therapist include maintaining continuity of care with the same physical therapist at each session, limiting the involvement of non-licensed personnel (i.e., aides or techs), and fostering interactions which promote collaboration between the patient and their therapist.
Thanks for reading!
Ernie
References
- Jensen GM, Gwyer J, Shepard KF. Expert practice in physical therapy. Phys Ther. 2000;80(1):28-43.