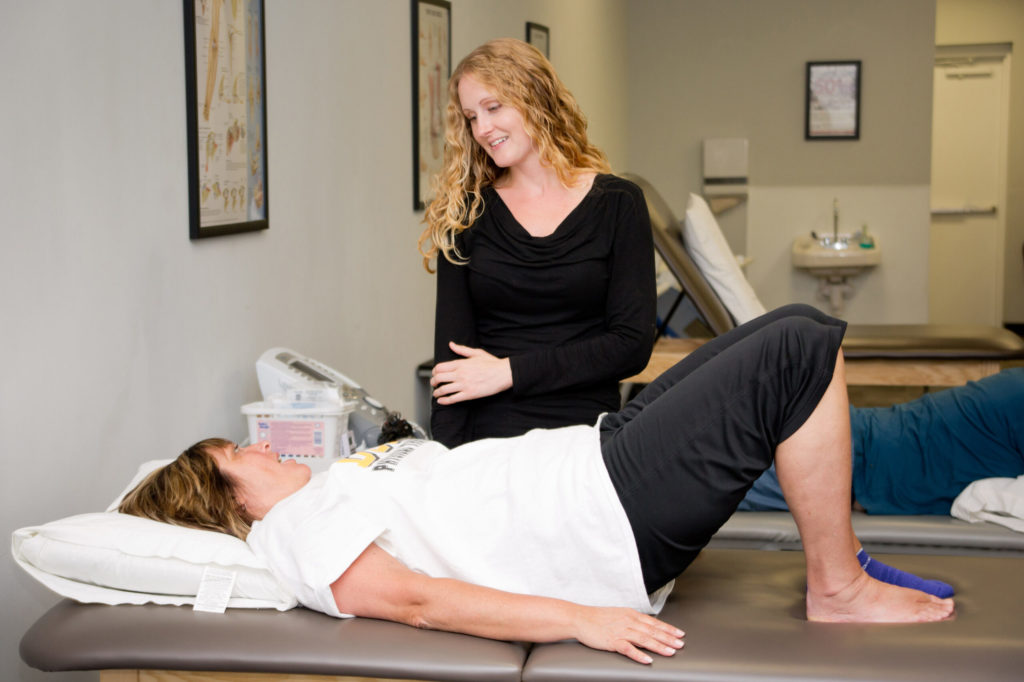
The leading cause of morbidity and mortality in the United States is chronic disease. Heart disease, stroke, cancer, diabetes, and…

Too many medical approaches in today’s society are dependent on others (therapists, doctors, etc) and include passive treatments (medications, injections,…

Resilience is the ability to recover from or adjust to misfortune or change. Successful recovery from injury requires resilience to…

Previously, I discussed the attributes of expert physical therapists. Experts share an inner drive for continual learning and improvement of their…

Recent changes in health care have placed increased pressure on physical therapists to become more efficient and effective with their…

Shared decision making between a patient and health care provider is linked with improved patient satisfaction, adherence to treatment, and…

The result of physical therapy treatment relies on the interplay between the technical ability, communication skills, and reflective capacity of…
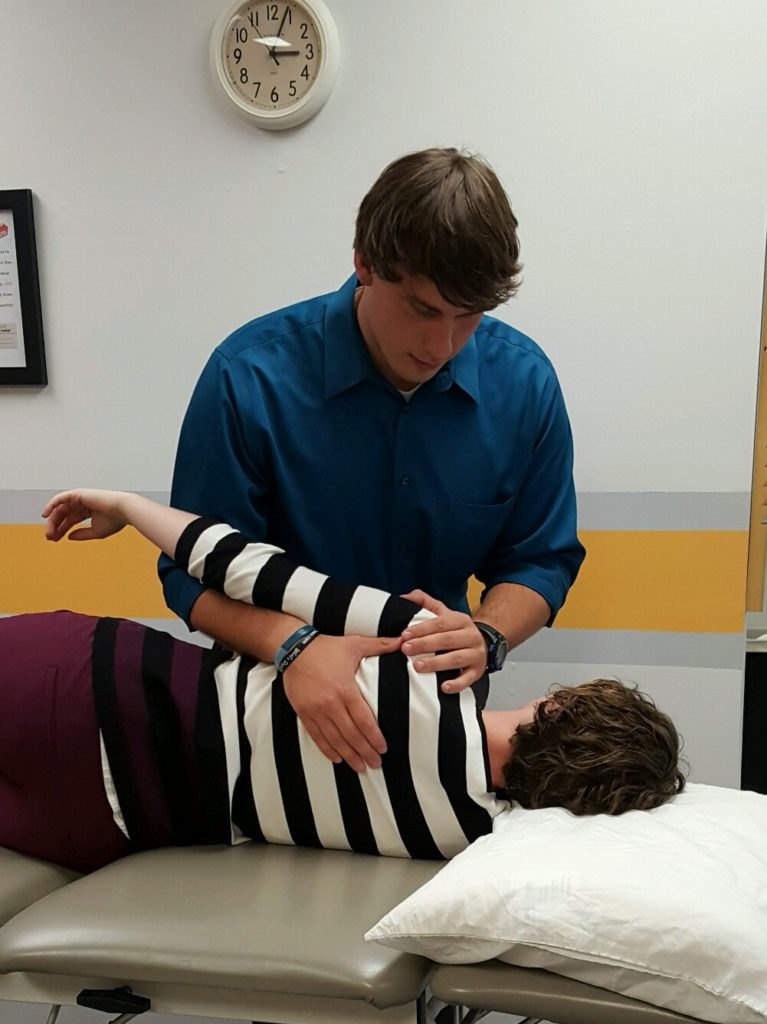
The therapeutic alliance refers to the collaboration between a patient and medical provider, their affective bond, and agreement on treatment…

The therapist-patient relationship, or alliance, is a critical factor in the success of your treatment plan. Therapeutic alliance refers to…
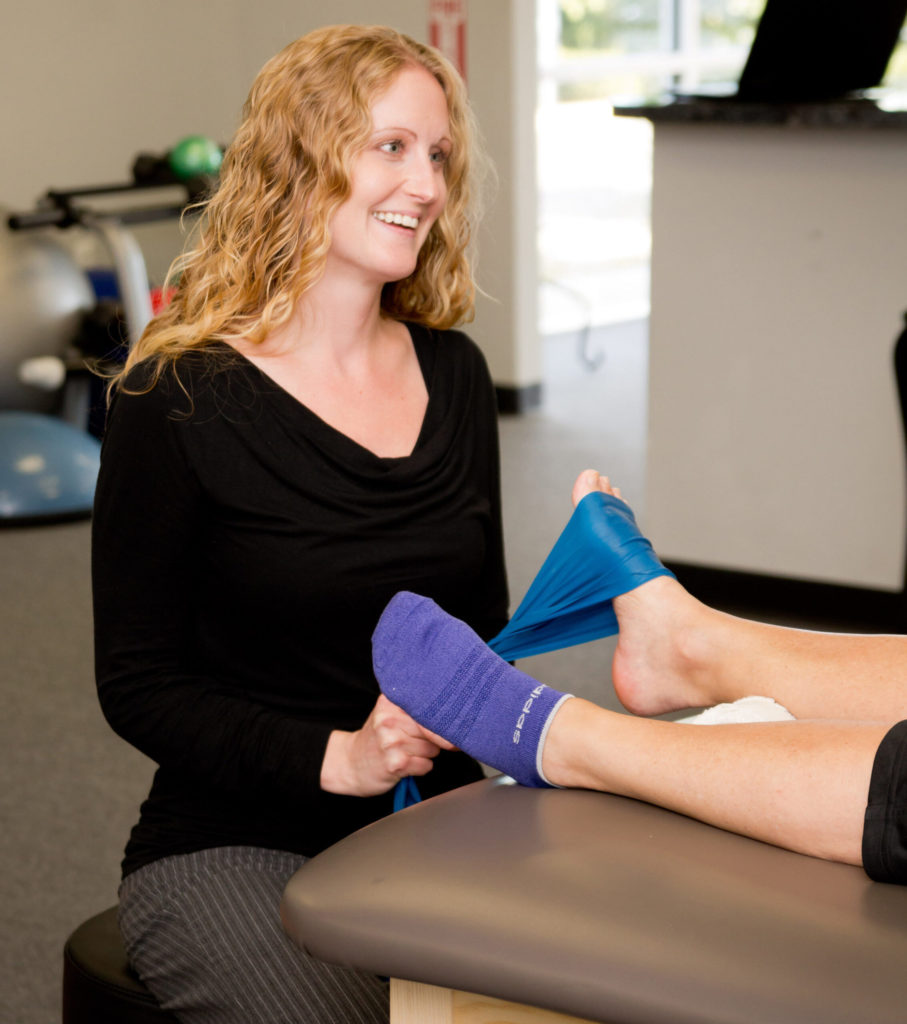
Health care in the U.S. is shifting towards a value-based system where patient satisfaction plays a key role in the…