We know how frustrating pain from knee arthritis can be. Due to pain and lost mobility, each year hundreds of…

Hip replacement surgery relieves pain for hundreds of thousands of people each year. However, some are disappointed because of persistent…

Reverse shoulder replacement is becoming an increasingly common surgery. If you are plagued by painful shoulder arthritis along with rotator…

Knee replacement surgery is a proven way to decrease pain from knee arthritis. Surgery also results in substantial improvements in…

Arthritis leads to more trouble walking and climbing stairs than any other muscle, joint, or bone problem. Treatment cannot “cure”…

Arthritis pain leads to reduced mobility and poor fitness. Pain from arthritis starts a vicious cycle. This includes reduced physical…

Your arthritis pain can be treated with exercise. Many forms of exercise have proven effective for arthritis. These include aerobic…
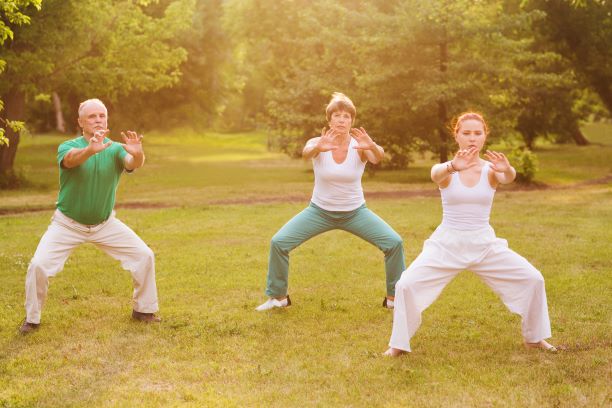
Are you having trouble walking, climbing stairs, or standing up from a chair? Is your knee or hip pain interfering…

If you are one of the millions of Americans bothered by hip or knee arthritis, this article is for you. …

Arthritis, according to the World Health Organization, is the single most common cause of disability in adults 60 years and…
